Bariatric surgery reduces risks of kidney failure, heart attack and death
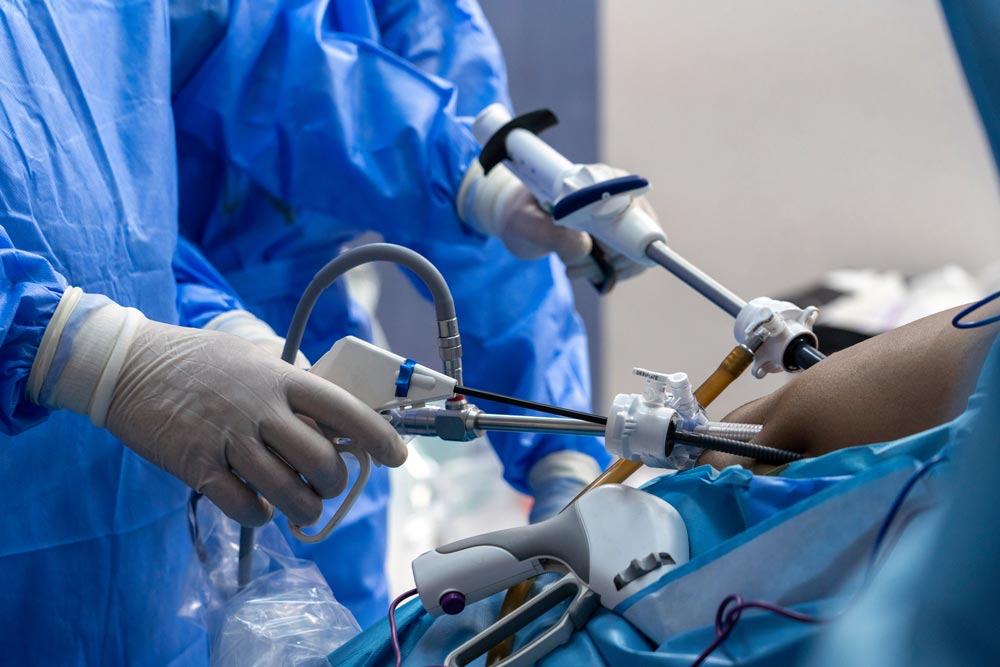
Researchers report that weight-loss surgery improves outcomes for patients with obesity and chronic kidney disease by significantly reducing the risk of kidney failure, major cardiovascular events and death.
The new findings were presented on May 5, 2026 at the annual meeting of the American Society for Metabolic and Bariatric Surgery (ASMBS).
“These findings show metabolic and bariatric surgery doesn’t just treat obesity, it fundamentally alters the course of chronic kidney disease and should be considered earlier in the disease process,” said lead study author Jerry Dang, MD, PhD, Associate Professor of Surgery at Cleveland Clinic Lerner College of Medicine of Case Western Reserve University. “With earlier intervention, we see slower disease progression, fewer patients advancing to kidney failure, better cardiovascular outcomes and greater access to life-saving transplants.”
As background, the authors noted that chronic kidney disease affects about 35.5 million Americans or about 1 in 7 adults. It is a leading cause of death in the United States. Obesity, diabetes, and hypertension are significant risk factors for the development of chronic kidney disease.
“The survival benefit of surgery patients observed in this study is extraordinary but not surprising,” commented ASMBS president Richard M. Peterson, MD, MPH. “These procedures are not simply about weight loss, they’re about changing the trajectory of chronic disease, preserving organ function and saving lives.”
The investigators in this retrospective study used data from the TriNetX Research Network (2010–2020), which included adult subjects with obesity and chronic kidney disease who had undergone sleeve gastrectomy or Roux-en-Y gastric bypass.
These subjects were matched 1:1 to subjects who had not undergone metabolic and bariatric surgery, with the matching based on demographics, comorbidities, baseline kidney function, and medication use.
Outcomes were recorded for a five-year period.
Primary endpoints included incidence of end-stage renal disease, dialysis initiation, kidney transplantation, cardiovascular events and all-cause mortality.
The investigators matched 4,481 metabolic and bariatric surgery subjects to 4,481 non- metabolic and bariatric surgery subjects.
They reported that compared to the non-metabolic and bariatric surgery group, the metabolic and bariatric surgery group had achieved significantly lower risks of end-stage renal disease (5.9% vs. 11.9%), dialysis dependence (4.1% vs. 9.0%) and composite cardiovascular outcomes (15.5% vs. 27.7%.)
Notably, kidney transplant rates were more than twice as high in the metabolic and bariatric surgery group (4.6% vs. 2.2%), and all-cause mortality was much lower (5.0% vs. 16.3%)
The authors concluded, “In this large real-world cohort, MBS [metabolic and bariatric surgery] was associated with substantial improvements in renal outcomes, kidney transplant access, cardiovascular health, and survival among patients with obesity and CKD [chronic kidney disease]. Prospective studies are needed to confirm these findings and inform clinical practice.”





