Oxygen therapy improves heart function in patients with long COVID
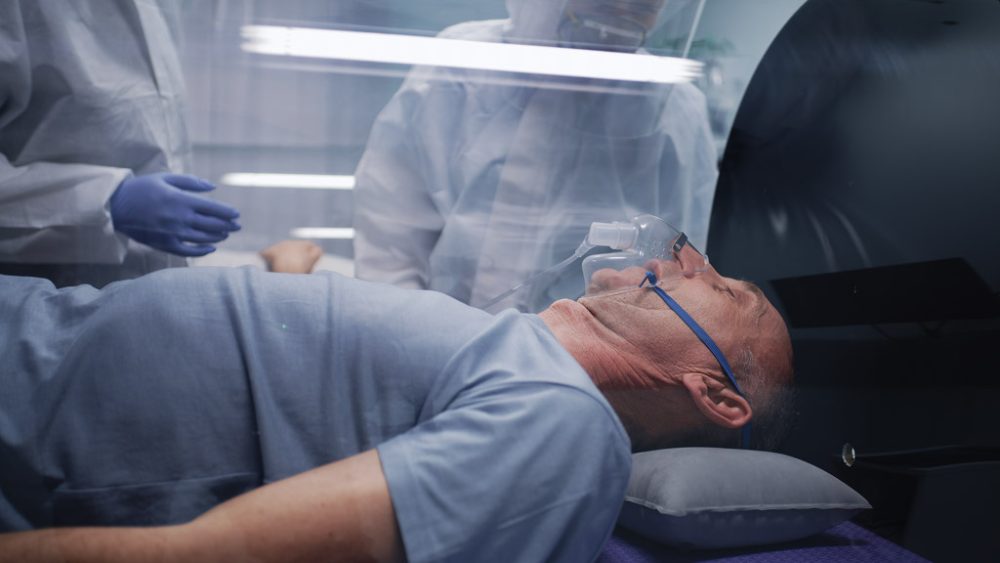
A small, randomised trial in patients with post-COVID syndrome has found that hyperbaric oxygen therapy (HBOT) promotes restoration of the heart’s ability to contract properly. The research was presented by a team from Israel at a scientific congress of the European Society of Cardiology (ESC) in Barcelona.
The study enrolled 60 post-COVID syndrome patients with ongoing symptoms for at least three months after having mild to moderate symptomatic COVID-19 confirmed by a PCR test. Both hospitalised and non-hospitalised patients were included. Severe COVID cases were excluded.
Patients were randomised to HBOT or a sham procedure in a 1:1 ratio. Each patient had five sessions per week over eight weeks, for a total of 40 sessions. The HBOT group received 100% oxygen through a mask at a pressure of 2 atmospheres for 90 minutes, with 5 minute air breaks every 20 minutes. The sham group breathed 21% oxygen by mask at 1 atmosphere for 90 minutes. All participants underwent echocardiography at baseline (before the first session) and 1 to 3 weeks after the last session.
Echocardiography was used to assess left ventricular global longitudinal strain (GLS), which is a measure of the heart’s ability to contract and relax lengthwise. It indicates how well the heart is functioning and can help detect early signs of heart disease. A healthy heart will have a GLS value of around -20% which means that the heart muscle is able to properly contract and relax in the longitudinal direction. Reduced GLS is an early marker that the heart is not able to contract and relax effectively.
‘The study suggests that hyperbaric oxygen therapy can be beneficial in patients with long COVID,’ said study author Professor Marina Leitman of the Sackler School of Medicine, Tel Aviv University and Shamir Medical Centre, Be’er Ya’akov, Israel.
‘More studies are needed to determine which patients will benefit the most, but it may be that all long COVID patients should have an assessment of global longitudinal strain and be offered hyperbaric oxygen therapy if heart function is reduced.’
At baseline, nearly half of study participants (29 out of 60) had reduced GLS. Of those, 13 (43%) and 16 (53%) were in the sham and HBOT groups, respectively. The average GLS at baseline across all participants was -17.8%. In the HBOT group, GLS significantly increased from -17.8% at baseline to -20.2% after the intervention. In the sham group, GLS was -17.8% at baseline and -19.1% after the sessions, with no statistically significant difference between the two measurements.
‘It was notable that almost half of long COVID patients had impaired cardiac function at baseline according to GLS despite all participants having a normal ejection fraction, which is the standard method for measuring the heart’s ability to contract,’ said Professor Leitman said. ‘This means that ejection fraction is not sensitive enough to identify long COVID patients with reduced heart function.’





