Robotic surgery is safer and improves patient recovery time
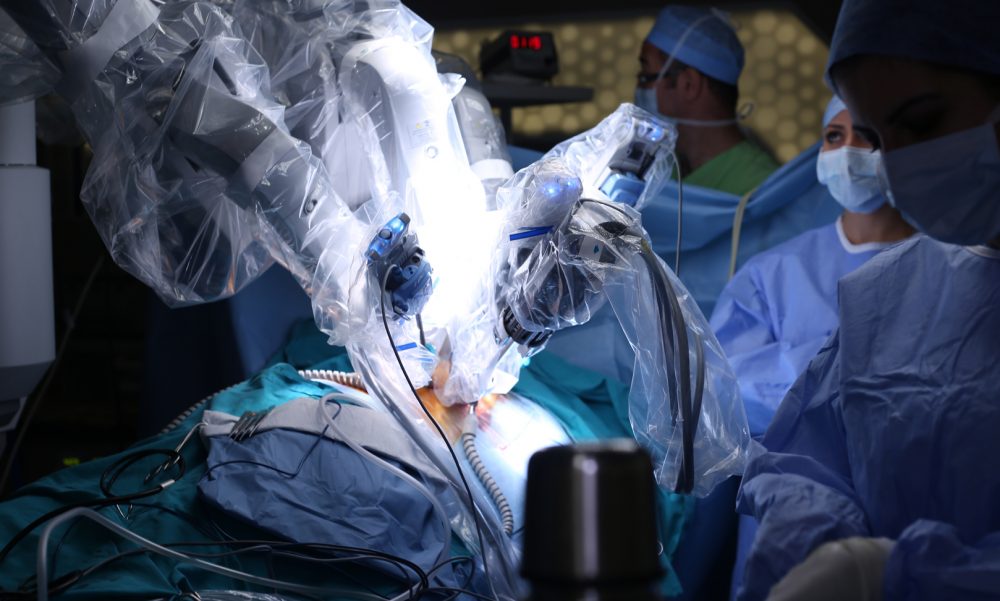
Robot-assisted surgery used to perform bladder cancer removal and reconstruction enables patients to recover far more quickly and spend significantly (20 per cent) less time in hospital, concludes a first-of-its kind clinical trial led by scientists at UCL and the University of Sheffield.
The study, published in JAMA and funded by The Urology Foundation with a grant from the Champniss Foundation, also found robotic surgery reduced the chance of readmission by half (52 per cent), and revealed a “striking” four-fold (77 per cent) reduction in prevalence of blood clots (deep vein thrombus & pulmonary emboli) — a significant cause of health decline and morbidity — when compared to patients who had open surgery.
Patients’ physical activity — assessed by daily steps tracked on a wearable smart sensor — stamina and quality of life also increased.
Unlike open surgery, where a surgeon works directly on a patient and involves large incisions in the skin and muscle, robot-assisted surgery allows surgeons to guide minimally invasive instruments remotely using a console and aided by 3D view. It is currently only available in a small number of UK hospitals.
Researchers say the findings provide the strongest evidence so far of the patient benefit of robot-assisted surgery and are now urging National Institute of Clinical Excellence (NICE) to make it available as a clinical option across the UK for all major abdominal surgeries including colorectal, gastro-intestinal, and gynaecological.
Co-Chief Investigator, Professor John Kelly, Professor of Uro-Oncology at UCL’s Division of Surgery & Interventional Science and consultant surgeon at University College London Hospitals, said: “Despite robot-assisted surgery becoming more widely available, there has been no significant clinical evaluation of its overall benefit to patients’ recovery.
“In this study we wanted to establish if robot-assisted surgery, when compared to open surgery, reduced time spent in hospital, reduced readmissions, and led to better levels of fitness and quality of life; on all counts this was shown.
“An unexpected finding was the striking reduction in blood clots in patients receiving robotic surgery; this indicates a safe surgery with patients benefiting from far fewer complications, early mobilisation and a quicker return to normal life.”
Co-Chief Investigator Professor James Catto, Professor of Urological Surgery at the Department of Oncology and Metabolism, University of Sheffield, said: “This is an important finding. Time in hospital is reduced and recovery is faster when using this advanced surgery.
“Ultimately, this will reduce bed pressures on the NHS and allow patients to return home more quickly. We see fewer complications from the improved mobility and less time spent in bed.
“The study also points to future trends in healthcare. Soon, we may be able to monitor recovery after discharge, to find those developing problems. It is possible that tracking walking levels would highlight those who need a district nurse visit or perhaps a check-up sooner in the hospital.”
“Previous trials of robotic surgery have focused on longer term outcomes. They have shown similar cancer cure rates and similar levels of long term recovery after surgery. None have looked at differences in the immediate days and weeks after surgery.”
Open surgery remains the NICE “gold standard” recommendation for highly complex surgeries, though the research team hope this could change.
Professor Kelly added: “In light of the positive findings, the perception of open surgery as the gold standard for major surgeries is now being challenged for the first time.
“We hope that all eligible patients needing major abdominal operations can now be offered the option of having robotic surgery.”
Rebecca Porta, CEO of The Urology Foundation said: “The Urology Foundation’s mission is simple — to save lives and reduce the suffering caused by urological cancers and diseases. We do this through investing in cutting-edge research, leading education and supporting training of health care professionals to ensure that fewer lives will be devastated.
“We are proud to have been at the heart of the step change in the treatment and care for urology patients since our inception 27 years ago, and the outcomes of this trial will improve bladder cancer patients’ treatment and care.”
Bladder cancer is where a growth of abnormal tissue, known as a tumour, develops in the bladder lining. In some cases, the tumour spreads into the bladder muscle and can lead to secondary cancer in other parts of the body. About 10,000 people are diagnosed with bladder cancer in the UK every year and over 3,000 bladder removals and reconstructions are performed. It is one of the most expensive cancers to manage.
Trial findings
Across nine UK hospitals, 338 patients with non-metastatic bladder cancer were randomised into two groups: 169 patientshad robot-assisted radical cystectomy (bladder removal) with intracorporeal reconstruction (process of taking section of bowel to make new bladder), and 169 patients had open radical cystectomy.
The trial’s primary end-point was length of stay in hospital post-surgery. On average, the robot-assisted group stayed eight days in hospital, compared to 10 days for the open surgery group — so a 20% reduction. Readmittance to hospital within 90 days of surgery was also significantly reduced — 21% for the robot-assisted group vs 32% for open.
A further 20 secondary outcomes were assessed at 90 days, six- and 12-months post-surgery. These included blood clot prevalence, wound complications, quality of life, disability, stamina, activity levels, and survival (morbidity). All secondary outcomes were improved by robot-assisted surgery or, if not improved, almost equal to open surgery.
This study, and previous studies, show both robot-assisted and open surgery are equally as effective in regards cancer recurrence and length of survival.
Next steps
The research team is conducting a health economic analysis to establish the quality-adjusted life year (QALY), which incorporates the impact on both the quantity and quality of life.
Journal Reference:
- James W. F. Catto, Pramit Khetrapal, Federico Ricciardi, Gareth Ambler, Norman R. Williams, Tarek Al-Hammouri, Muhammad Shamim Khan, Ramesh Thurairaja, Rajesh Nair, Andrew Feber, Simon Dixon, Senthil Nathan, Tim Briggs, Ashwin Sridhar, Imran Ahmad, Jaimin Bhatt, Philip Charlesworth, Christopher Blick, Marcus G. Cumberbatch, Syed A. Hussain, Sanjeev Kotwal, Anthony Koupparis, John McGrath, Aidan P. Noon, Edward Rowe, Nikhil Vasdev, Vishwanath Hanchanale, Daryl Hagan, Chris Brew-Graves, John D. Kelly, E Ruth Groves, Louise Goodwin, Jayne Willson, Phillip Ravencroft, Stephen Kennish, Derek J Rosario, Carol Torrington, Rajesh Nair, Ramesh Thurairaja, Sue Amery, Kathryn Chatterton, Samantha Broadhead, David Hendry, Abdullah Zreik, Sunjay Jain, Steve Prescott, Hannah Roberts, Angela Morgan, Chris Main, Elspeth Bedford, Lorraine Wiseman, Bernice Mpofu, Claire Daisey, Michelle Donachie, Jon Aning, Lyndsey Johnson, Carol Brain, Constance Shiridzinomwa, Martin Ebon, Alexander Hampson, Roisin Schimmel, Scott Horsley, Sayyida Nembhard, Clare Collins, Jemma Gilmore, Faith Wilson, Louise Peacock, Sheena Lim, Rhosyll Gabriel, Rachael Sarpong, Melanie Tan. Effect of Robot-Assisted Radical Cystectomy With Intracorporeal Urinary Diversion vs Open Radical Cystectomy on 90-Day Morbidity and Mortality Among Patients With Bladder Cancer. JAMA, 2022; DOI: 10.1001/jama.2022.7393





