More severe stroke patients should receive palliative care consultations
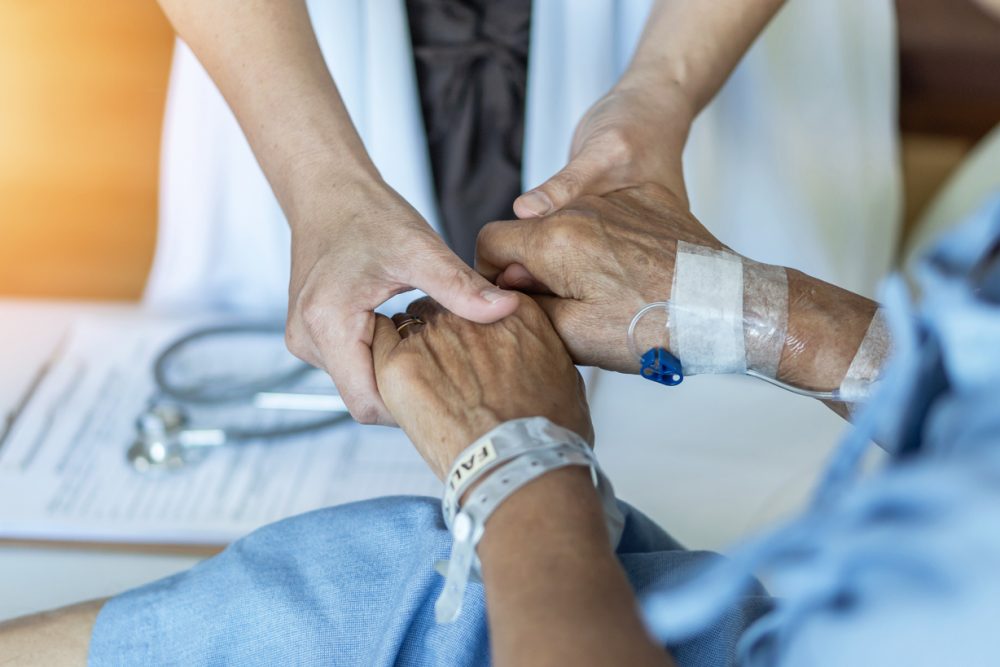
Only 20 percent of patients being treated in the hospital for severe stroke received a palliative care consultation, and only 43 percent of patients who died in the hospital met with a palliative care team, according to a new study from Regenstrief Institute and Indiana University. Study authors believe more people should be receiving these consultations that outline care options, clarify care preferences and potentially reduce prolonged suffering.
“Stroke is a major life crisis where patients and their families need to make major decisions, and they need significant support. Palliative care teams provide that,” said senior study author Alexia Torke, M.D., M.S., Regenstrief research scientist and professor of medicine at Indiana University School of Medicine. “When a person has a very severe stroke, they may not recover the ability to eat or breathe on their own. The palliative care team can help families and patients determine what they view as an acceptable outcome and how aggressive they want to be with treatment to reach that outcome. Sometimes, the patient and family may choose to receive comfort care rather than a feeding tube or ventilator.”
Palliative care teams communicate treatment options for patients and their families, explaining the best, worst and most likely outcomes for each. Care focused on comfort rather than life-prolonging measures is included in these discussions. They guide patients and families in defining values, preferences and goals for treatment, supporting them in making the appropriate decision to achieve an outcome that is acceptable to the patient.
The research team looked at the health records of more than 1,200 stroke patients in four health systems in Indiana to determine how many patients received the consultations. Older and sicker patients were the most likely to meet with the palliative care teams. And patients who received the consultation were more likely to move to a plan focused on comfort measures.
“We found that palliative care is being used appropriately, however, there are some missed opportunities,” said first author Amber Comer, PhD, J.D., associate professor in the IU School of Health and Human Sciences. “For example, more than half of the stroke patients who died in the hospital did not meet with the palliative care team. Some of these patients may have received more treatment than they preferred because they did not receive support and guidance in defining preferences and goals.”
The next focus of research in this area is to look at the goals of these palliative care conversations. Research scientists are also working to create a palliative care screening tool to help clinicians determine which patients are good candidates for palliative care consultations.
“Palliative and End-of-Life Care After Severe Stroke” is published online in the Journal of Pain and Symptom Management. This research received a grant from the National Palliative Care Research Center.
In addition to Drs. Comer and Torke, authors on the paper are Linda Williams, M.D., Regenstrief Institute, VA Health Services Research and Development Center for Health Information and Communication, IU School of Medicine; Stephanie Bartlett, P.T., IU School of Health and Human Sciences; Claire J. Cruetzfeldt, M.D., University of Washington; James E. Slaven, M.S., IU School of Medicine and Robert Holloway, M.D., MPH, University of Rochester School of Medicine.
JOURNAL
Journal of Pain and Symptom Management
DOI
10.1016/j.jpainsymman.2021.12.032





