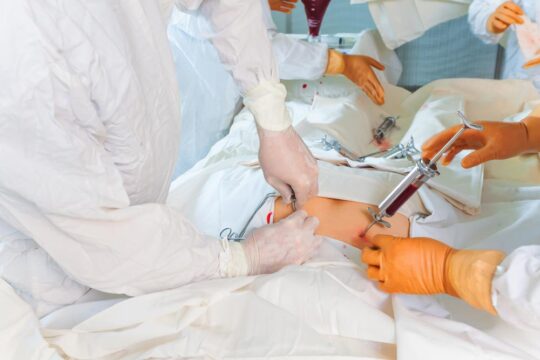
Ablation possible when steroid injections fail
Patients with low back pain who don’t respond robustly to intra-articular steroid injections may still be candidates for treatment with radiofrequency ablation (RFA), researchers said here.
Those with sacroiliac joint pain who had at least a 25% response to the injections still appeared to benefit from RFA of the lateral branches, Jianguo Cheng, MD, PhD, of the Cleveland Clinic in Cleveland, and colleagues reported at the American Academy of Pain Medicine meeting.
“The duration of pain relief after radiofrequency ablation … is independent of the degree of pain relief within the range of 25% to 100% after sacroiliac intra-articular steroid injections,” Cheng said during an oral presentation. “Don’t disqualify a patient from radiofrequency ablation if they only achieved 25% to 49% relief from steroid injections.”
Therapeutic options for spinal pain, particularly at the sacroiliac joint, are lacking because clinicians don’t fully understand the mechanisms of the pain, Cheng explained. Intra-articular steroid injections have been commonly used, but the length of pain relief they provide varies.
Traditionally, the degree of pain relief from steroid injections has been used to determine if patients would be good candidates for RFA of the lateral branches that innervate the sacroiliac joint. RFA of the lateral branches is often considered only if the patient had more than 50% pain reduction from intra-articular steroid injection.
Cheng’s group conducted a retrospective study of 80 patients who underwent pre-operative intra-articular steroid injections RFA from January 2006 to June 2009 at the Cleveland Clinic.
The vast majority (75%) of these patients had at least 50% pain relief from the injections, while the rest had a response of 25% to 49%.
Cheng said patients with the more robust responses had the following characteristics:
- Older age
- More likely to have pain radiating to the leg
- More likely to have gradual onset pain
- Less likely to have pain with extension or axial rotation
Overall, they found that the degree of pain relief within the range of 25% to 100% from sacroiliac joint intra-articular steroid injection did not predict the outcomes of RFA. The duration of pain relief post-RFA of the lateral branches was independent of the degree of pain relief within the range of 25%-100% after steroid injections.
After adjusting for variables such as age, modes of pain onset, multiple pain complaints, and responses to extension or axial rotation of the lumbar spine in the multivariable proportional hazards model, the difference in duration of post-RFA pain relief between the groups was not significant (hazard ratio 0.96, 95% CI 0.49 to 1.90, P=0.91).
However, Cheng noted that at six months after RFA, the overall efficacy of the procedure in their patient population appeared to be lower than in previous studies. That may be because the study cohort was older, had a higher rate of previous spine surgery, had a higher rate of opioid use, and had greater pain complaints.
Clinicians who are considering RFA in patients who demonstrate a lower response to steroid injections should consider a physical exam as well as the patient’s history before proceeding.
He added that there aren’t many alternative treatments for patients who are denied RFA by their insurance companies. “Many people end up on [long-term] opioids, which often creates possible opioid-related problems.”
Disclosure:
The study was partly funded by the Anesthesiology Institute of Cleveland Clinic.
The researchers reported no conflicts of interest.
Reference:
Cheng J, et al The degree of pain relief from intraarticular steroid injection of the sacroiliac joint does not predict the outcomes of radiofrequency ablation of the lateral branches AAPM 2012; Abstract 136.