IASLC 2011 Report – Re-evaluation of the management of malignant pleural mesothelioma
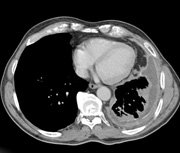
by Dr Sunil Upadhyay – Malignant Pleural Mesothelioma (MPM) is of insidious onset and almost uniformly a fatal disease. Around 90% of the patients can be linked to asbestos exposure. The management outcome of MPM remains dismal. The majority of the patients present with advanced disease, are elderly and have multiple co-morbidities. The common prognostic factors identified are age, sex, performance status, stage and histology. Various treatment modalities used in the management of MPM have included surgery in an extremely small number of patients with or without chemotherapy and/or radiotherapy. Intra-pleural chemotherapy followed by surgery and neo-adjuvant chemotherapy has also been tried but failed. Other novel multi-modality treatments being looked at are intra-pleural photodynamic therapy (PDT) and intra-pleural hyperthermic chemo-perfusion plus surgery. Mature data are appearing from multiple trials.
The role and extent of surgical procedures is terribly controversial. As far as surgery for MPM is concerned, it remains to be standardised. It is often difficult to quantify the location and extent of the disease using current available investigational procedures. We need to question what is the ideal surgery and is maximal cyto-reduction optimal in the surgical management of MPM.
As far as the pleurectomy and de-cortication is concerned, actually it is a marginal resection instead of a maximal resection. Extended pleurectomy/decortication which includes diaphragm and/or pericardium resection is rarely performed. These procedures are preferred for patients with early stage disease or poor pulmonary reserve so that their lung can be spared and morbidity minimised. On the other hand when a thick layer of pleura surrounds the pleural space, the more extensive extra pleural pneumonectomy (EPP) involving an en bloc resection of the lung, visceral and parietal pleura, pericardium and hemi-diaphragm has to be the preferred choice but by an experienced cardiothoracic surgeon. The surgical procedure of choice depends on meticulous patient selection, co-morbidities, extent of the disease and adjuvant therapies following surgery. The surgical outcome is highly dependent on the expertise of the surgeon. It is no good to do pleurectomy or EPP without adjuvant therapy in 2011. Adjuvant chemotherapy has dramatically improved the median overall survival to 30 months in most of the studies by stage and operation. For early stage cases, with the use of postoperative adjuvant treatment median survival of up to 44 months has been reported.1,2 Moreover, whether adjuvant therapy had been delivered or not, pleurectomy was at least equivalent to EPP in both early and late stage.
The use of adjuvant therapy, epithelial histology, female gender and early stage are associated with longer survival. There is no advantage to use either pleurectomy or EPP alone for survival; however the trend was in favour of pleurectomy with reduced risk of death. Both these operations are suboptimal in preventing relapse without the use of adjuvant therapy. David Sugarbaker was the first to use multimodality therapies in a scientific way (Click here for table of EPP, adjuvant chemotherapy and adjuvant radiotherapy).
The current gold standard chemotherapy for MPM is cisplatin and pemetrexed. However, if the most important predictor of survival after induction therapy is adjuvant chemotherapy, we need to personalise the treatment by looking at the stage of the disease, molecular behaviour and genomic markers (Thymidylate Synthase, ERCC1, RMM-1) of the tumour to optimise the use of chemotherapy. Sequencing, gene profiling and the role of biological agents needs to be investigated to maximise the outcome. The published results of the commonly practiced sequencing of neo-adjuvant chemotherapy followed by EPP/pleurectomy and adjuvant radiation trials continues to show the average median survival of 20 months and 30 months survival of 30%, which is no better compared to the adjuvant data. Sadly, the use of intra-operative hyperthermic cisplatin and other currently available cytotoxic agents has been disappointing. (Harvey Pass, Educational session E01.2).
References:
1. Sugarbaker D, Richards WG, Godleski JJ, Yeap BY, Corson JM et al. Cancer 2010; 116: 1510-17
2. Rusch VW, Venkatramen ES et al. Ann Thoracic Surgery 1999: 68: 1799-1804





